INTRODUCTION
This booklet has been compiled by Melbourne Hip and Knee to help you better prepare you for knee realignment surgery, and to provide guidelines for post-operative recovery, care and rehabilitation. The long term goal of knee realignment surgery is to provide pain relief, return you to normal daily activities and ensure you have an enhanced quality of life.
HOW DOES THE KNEE WORK?
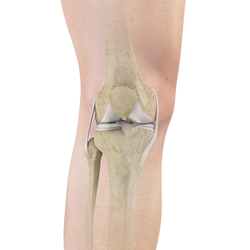
The knee joint is made up of three bones, these are, the femur (thighbone), the tibia (shinbone), and the patella (kneecap). The knee is a hinge joint, however, it has a complex rotational component that occurs with flexion and extension of the knee. The knee is held together by muscles, ligaments and other soft tissue, that enables it to bear a significant weight. Cartilage is located inside the knee joint and provides shock absorption during weight bearing activities (such as walking or climbing stairs).
WHAT IS ARTHRITIS?
As we get older the cartilage in our joints becomes more brittle and is likely to wear out or degenerate. This can lead to osteoarthritis, which is the wearing out of the lining (articular) cartilage, and is the most common cause for a total knee replacement. Due to the osteoarthritis, the cartilage in the knee breaks down and the result is a badly damaged joint surface, often, with bone rubbing on bone. This can become stiff and may become deformed or angulated. In the early stages of arthritis, pain is normally mild and only felt after exercise. It is usually a dull ache and may be associated with some swelling. As arthritis progresses the pain will become constant and more severe. It may be painful at rest and wake you up at night. Some patients due to the shape of their leg or due to an injury or accident develop arthritis in only one part of the knee.
WHAT NON SURGICAL TREATMENT IS AVAILABLE?
If you have arthritis in your knee, the first step is to try simple treatments such as taking painkillers and anti-inflammatories and gentle knee exercises. Weight loss can also significantly improve symptoms. Used in combination, these treatments can improve your pain and level of function significantly and you may not need anything else at this stage.
WHY HAVE KNEE REALIGNMENT SURGERY?
If you have tried all of the above, and you are still getting significant pain and stiffness that is preventing you from doing the things you want to do, and your arthritis is limited to one part of the knee you may be a candidate for knee realignment surgery. This is performed if you are considered too young or active for a knee replacement, or the arthritis is not at the advanced 'bone on bone' stage. The aim is to change the angle of the leg to take the stress off the worn part of the knee and onto the normal (not worn) part and allow return to activity and delay the need for a knee replacement.
Patients who are bow legged wear out the inner (medial) part of the knee, while patients who are knock kneed wear out the outer (lateral) part of their knee.
KNEE REALIGNMENT SURGERY – ABOUT THE PROCEDURE
In knee realignment surgery the aim is to take the stress off the worn part of the knee and move it to an area that is not worn. Knee realignment surgery typically takes between one to one and a half hours to complete. Surgery is performed under sterile conditions in the operating room under spinal or general anesthetic (you will be asleep). You will be on your back and a tourniquet applied to your upper thigh to reduce blood loss.
In the knee realignment procedure, the bone is cut 80% of the way across and then bent by a predetermined amount and fixed in place with a metal plate and screws. Sometimes bone is used to fill in the gap created by cutting and bending the bone.
In patients who are bow legged the tibia is normally cut just below the knee (High Tibial Osteotomy).
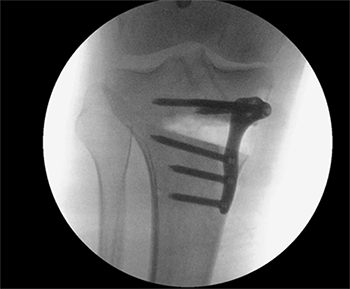
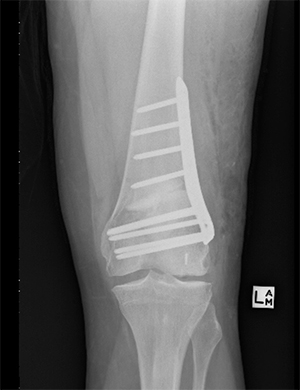
In patients who are knock kneed the femur is normally cut just above the knee (Distal femoral Osteotomy)
WHAT DO I NEED TO DO TO PREPARE FOR KNEE REALIGNMENT SURGERY?
Once you and your surgeon have decided to proceed with surgery, there are several steps to be taken to ensure your procedure goes smoothly.
- X-rays and Scans
In order to accurately measure the degree of correction that is required, you will need to have special x-rays taken of your legs from the hip all the way down to the ankle. The x-rays are taken with you standing as straight as you can.
You may also need to have an MRI scan or CT scan to help plan your surgery. If your surgeon has requested these please organize to have them as soon as possible.
- Start pre-operative exercises
It is important to be as flexible and strong as possible before undergoing knee realignment surgery. Many patients with arthritis favour the pain free leg, as a result muscles can become weaker, making recovery slower and more difficult. It is important therefore, to begin an exercise program before surgery to learn and practice the exercises that will improve your strength and flexibility making recovery easier and faster. Melbourne Hip and Knee offers pre and post-operative physiotherapy sessions onsite at our main rooms in Hawthorn East. To book an appointment call , alternatively, if you have a regular physiotherapist they will be able to get you on track.
- Make arrangements for help around the house
It is important to have your house ready for when you return home. You may need to modify sleeping arrangements if they are up a lot of stairs. You should also put things that you use often within easy reach, remove cords or obstructions from walkways, arrange for someone to walk the dog and collect the mail.
- Stop smoking
Stop smoking as long as possible prior to surgery. Smoking delays your healing process. It reduces the size of your blood vessels and decreases the amount of oxygen circulated in your blood. Smoking greatly increases your chances of getting an infection of your prosthesis or the wound breaking down. It also significantly slows the healing of the bone and makes it much more likely that the bone won’t heal. Smoking can also increase clotting, which can cause problems with your heart. Smoking increases your blood pressure and your heartrate. If you quit smoking before you have surgery, you will increase your ability to heal.
WHAT DO I NEED TO KNOW ABOUT GOING TO HOSPITAL?
- Arrival: You will be asked to attend the hospital approximately two hours before the anticipated time of your operation. There are several stages to your admission process and this ensures that adequate time is available.
- Fasting: Fasting is important to ensure your procedure can occur, and it includes refraining from all food and fluids, including water, chewing gum, mints or lollies. You will be asked to fast for at least six hours before your surgery
- Medications: Please bring all current medications with you to the hospital. Please check with your anaesthetist to determine if you should take your regular medications on the day of surgery.
- X-rays/Scans/Imaging: please bring all that you have to the hospital. This includes the actual scans (not just the reports).
- Luggage: space is limited so avoid bringing unnecessary items. We strongly recommend you do not take valuables to hospital, no liability for loss, theft or damage of valuables will be accepted by hospitals.
WHAT HAPPENS WHEN I ARRIVE AT HOSPITAL?
The following processes will occur:
- Clerical admission- you will be initially admitted by a clerical staff member at the hospital. They will check all of your administrative details and take any payments due.
- Clinical admission- you will then undergo a clinical admission where a nurse will discuss your medical history, this may include recording your height, weight and blood pressure. If any blood tests or other investigations are required they will be taken at this time. You will be changed into a theatre gown.
- Anaesthetic review- your anaesthetist will visit you prior to your surgery to explain the type of anaesthetic you will be receiving.
- Surgeon- your surgeon will again explain the procedure you are about to undergo. They will mark the correct part of your body where the procedure will happen. You will also sign surgical consent.
WHAT HAPPENS AFTER MY PROCEDURE?
- Recovery
When you wake you will be in the recovery room with intravenous drips in your arm and a number of other monitors to check your vital observations. You may have a button to press for pain medication. Once stable, you will be taken to the ward. The post-operative protocol is surgeon dependant. You will start moving your knee soon after surgery. You are encouraged to begin physiotherapy exercises straight away and to bend and straighten the knee to help regain muscle strength. The day after your surgery the physiotherapist will supervise you using crutches. You will not be able to put all your weight on the leg. Normally you are restricted to Touch weight bearing for 6 weeks after surgery. This means you can touch your foot to the ground for balance but not put any weight through it.
- Dressings
You will initially have a large outer bandage on your knee. This will usually be removed about 24 hours after your operation. There will be a smaller waterproof dressing beneath this which should remain in place for two weeks. Dissolvable stitches are used.
- Going Home
Normally you would be in hospital for two to three days. You will be discharged on crutches for 6 weeks. Please ensure you arrange for someone to pick you up.
- Pain Management
You should take regular painkillers and ice the knee regularly for the first few weeks to make sure the knee feels comfortable, and also to allow you to do your physiotherapy exercises. You should wear compression stockings (day and night) and you may be asked to take daily blood thinners for one month after surgery to decrease the risk of developing blood clots. It takes several weeks for the pain to settle down and it can be several months before it really feels normal.
- Post-operative appointment
You will usually have a post-operative appointment booked to see your surgeon approximately two weeks after surgery. Your appointment information is on your admission letter. Please call Melbourne Hip and Knee if you are unable to locate this information. If you are still in a rehabilitation facility when you are due to have your appointment, please call us to reschedule. After 6-8 weeks, and then after 3-4 months, you will have further follow up appointments with new x-rays to look at the bone healing.
Physiotherapy
You will have physiotherapy each day in hospital and you should continue to see a physiotherapist after you leave hospital. If you have seen a physiotherapist prior to surgery you should return to them after the surgery for follow up exercises.
Returning to activity
You will need to use crutches for 6 weeks following surgery, during this time you will not be allowed to put much weight through your operated leg.
Driving. If surgery is on your left knee and you drive an automatic car then you can drive when you are off all strong painkillers and can easily get in and out of the car. This may be as soon as 1-2 weeks after your operation. If you have left knee surgery and you drive a manual car it will take at least 6 weeks for the knee to be strong enough to drive,
If you have right knee surgery, then you will not be able to drive for 6 weeks or longer.
Work. If you have a desk job and you can get to and from work you may be able to return to work as early as 2 weeks after surgery although it often takes 3-4 weeks. You can work from home as soon as you are off strong pain killers. For patients who perform more physical work it will take 2-3 months before you are able to return to work and you may have to stay on light (restricted) duties for a couple of months.
Walking unaided. You will be on crutches for 6 weeks and then will take a further few weeks to be able to walk unaided.
Sport (swimming/hydrotherapy). You can start hydrotherapy as soon as the wound has fully healed. this is normally around 3 weeks after surgery but make sure you get the clearance from your surgeon first. As part of your rehabilitation you may start on an exercise bike after 2 months. It will normally take a couple more weeks before you are able to ride a normal bike. Returning to sport will take at least 6 months and may not be possible for all patients
Sex. Once your wound has healed and you are comfortable you are able to return to sexual activity. Positions where you are resting on the knee or have the knee bent a lot may be difficult.
WHAT ARE THE RISKS OF HAVING KNEE REALIGNMNT SURGERY?
- Anaesthetic
There are risks associated with the anaesthetic, including the possibility of heart attacks, strokes and breathing difficulties. The chance of these occurring is generally very low.
- Infection
There is a risk of the knee getting infected. This occurs in 1 in 100 operations. If the knee gets infected, you may need further operations to wash it out. If the infection is severe, the metal fixation may need to be removed and then replaced again once the infection is cured.
- Nerve Injury
There is a small risk of injury to the nerves and blood vessels around the knee. The chance of any major injury is extremely low. You may always develop a small patch of numbness on the side of your cut. This is because one of the nerves that provides feeling to that part of the knee always gets cut when the skin is incised.
- Blood Loss
It is rare to need a blood transfusion after this surgery.
- Blood Clots (DVT)
As mentioned above, there is a risk of developing clots in the legs which can then go to the lungs. You may be given special stockings to wear and blood thinning medication to reduce this risk. It is also important to do you exercises to increase blood flow to the lower leg.
- Pain
While the aim of surgery is to improve your pain some patients report that the knee is still a little bit stiff and uncomfortable after the surgery. The knee will not bend as well as a knee that has never had any problems and may be swollen for a few months.
If you have any further questions, please ask your surgeon.

